Playing Fast and Loose with Euthanasia

Bone Cancer and Bone Heads
Irma is a lively senior Golden Retriever patient of mine, suffering from bone cancer on her left upper arm. She lived a healthy life before this, so I only got to meet her after this calamity called osteosarcoma was diagnosed in October 2014.
Irma’s one of those dogs who’s friendly to anyone she meets, who knows no strangers. Her face turned white when she was only four years old, and now there’s a whole lot of white hairs mingled into her coat at age 12.
Luckily for Irma, she didn’t experience too much conventional medicine, though she did have some vaccinations up until age eight. More telling, when I asked Mike about the possibility of any injury earlier in life was this:
“When she was a young pup, she fearlessly leapt off an 8 foot ledge, surprising the friend who took her for a walk. She limped for a bit after that, and that limp reminded me of this limp she shows now.”
Interesting. Research shows that a high percentage of cancer cases had an earlier history of traumatic injury, 50% or more according to one of my teachers.
Rx: Death, Based on Radiograph. Patient Ignored.
Irma went in to get radiographed last week to see how her bone cancer looked. It’d been there in her left arm for a few months by now, and while she limped, she was every bit the engaged, happy, hungry and even playful dog she had been for years. Her pain was being managed with a couple of well known pain meds.
The radiographs showed the cancer had advanced. That’s not uncommon in osteosarcoma. Here’s what that looked like to the x-rays that were beamed through her arm to visualize the brute:
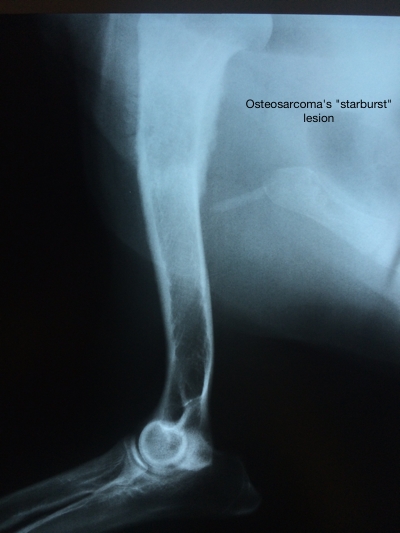
See where the borderline of Irma’s humerus gets fuzzy up near the top? That’s the cancer, and the bone’s abnormal growth in this disease.
In discussing her findings, the conventional vet suggested the limb could fracture and euthanasia should be considered in the next couple of days. Mike and Shelley, hearing this, were taken aback.
I was called to weigh in on this idea, as was a Canadian vet Irma saw briefly when she was there for a spell.
We both agreed: unless Irma is clearly giving up or in intractable pain, it’s premature to get her scheduled for euthanasia. She was nowhere close!
[Now, even 10 days later, as I’m writing this, Mike stopped in to pick up some Irma supplements and reiterated how glad they were in not heeding this advice. “She’s still happy to be alive!”]
Irma is still wagging for each meal, cleaning up her raw food like there was no tomorrow, and very involved with her owners and their kids. Earlier, Mike sent me a video he’d taken on that scary day. There’s Irma, lying on her back in the living room, happily wriggling and even reaching playfully for her tail.
Put her to death? That’s a very final decision. There may come a time for it, but we’ll all know when that time comes.
What’s Wrong with This Picture?
There are some surprising attitudes on Dr. WhiteCoat’s part that drive euthanasia decisions. They unfailingly catch me off guard and often make me furious. There’s no returning from that decision once it’s made. While I see its place in the grand scheme of things, it needs to be the final card played. If it’s played at all.
The recommendations that most rub me wrong are the ones based on the disease instead of the patient. The gross incongruence in these situations is jarring. I’ve had cat patients whose owners were told, “She’s positive for feline leukemia. We should euthanize her.” After homeopathic treatment, these guys inevitably have thrived, often for years. Same with FiV, feline AIDS.
Irma’s cancer is a another example. Those radiographs show her pathology clearly, and make it look like recovery is unlikely. I’d agree, and we went into her homeopathic treatment knowing those odds.
The best we seem to be able to achieve with homeopathy is curing about 10% of our patients who are living with a malignancy. The other 90% live a better quality of life than what conventional medicine offers, especially chemotherapy. And, when it’s time to die, the homeopathically treated ones can often die peacefully at home on their own. That stands in stark contrast to those who’ve undergone chemo, radiation, or surgery, who often need euthanasia in the end to relieve a very difficult state.
Dogs with this very disease have largely done well after amputation, as well.
So, I wonder if Dr. WhiteCoat’s thinking becomes,
- We’re going to lose her anyway, so let’s wrap this up.
- This is impossible to cure but I need to do something.
- I’m a doctor. I can control even death with my medicines!
But what about that happy dog who’s walking around your exam room, getting pets from anyone who offers them, and still has a happy attitude and an eager appetite? Can you really, in your heart of hearts, think it’s time to put this animal to death?
When It’s Clearly Euthanasia Time
It’s not always easy to call it, but there are some infallible markers in my experience that say, “It’s time.” I’m talking about end stage disease in the following examples, where the owners and the doctors know that recovery is impossible, short of a miracle.
- 1. It’s impossible to rest or sleep uninterruptedly.
These animals are continually shifting position. It just seems the pain of their condition is inescapable. If they can’t nap or sleep for hours, life is hell and it’s time to help them transition with euthanasia.
- 2. Vocalization.
The level of pain and discomfort is at the point where moaning or barking or whining is now a regular part of every day, multiple times a day. When they are calling out like this, it is clear: it’s time to offer the gift that euthanasia is.
Less Clear, But No Shame
There are also times when I’ve offered euthanasia as an option when the following line up:
- The disease is clearly not going to be cured, even with the best homeopathy has to offer.
- The animal’s quality of life has really deteriorated:
- Incontinence is the norm, not the rare exception. Every elimination is unpredictable and lands where ever the animal is at the moment.
- Paralysis makes the simplest act, like standing to eliminate, impossible. I see this in the German Shepherds and others who have spinal disease: normal from the waist up, but completely paralyzed in their lower half. They are often the victims of scalding from dribbling urine and/or stool.
- Multiple senses have failed, so the poor beast no longer sees nor hears her world. Touch startles her.
That’s not to say these animals must be euthanized. There are owners who would do what ever it takes in terms of supporting these creatures and don’t mind cleaning up after them on a regular basis. I’m only suggesting that I will never object to euthanasia if the owner sees it as an option in advanced terminal conditions like these.
It’s exhausting, caring for an animal in this stage, and I think euthanasia is a very acceptable decision at this point. That’s especially true in animals you’ve known to be extremely clean in habit, or who would never, ever, even with a bursting bladder, eliminate in the house. How must they feel now? We can only guess, but there could well be an emotional price exacted daily when they are no longer in control.
How about you? Tell us in the comments how you’ve dealt with this often difficult time at the end of life . And tell us if you’ve had to ignore a recommendation for euthanasia that was clearly premature.




@Susan Capuano, I went to 3 or 4 vets, they all said it was too late. All they offered was comfort meds, tramadol, rimadyl, neurontin etc. She had 1 month left, period.
Hemangiosarcoma is a very aggressive form of cancer, it often shows no symptoms till it has metastasized.
Dogs tend to be stoic and hide pain, in the wild being sick is a weakness they can’t afford, because the pack members will turn on them. This dog was walking 5 miles a day with me up until a month before she died. She never had so much as a cold before this thing struck at 9 years, 8 months. She was a beautiful Welsh Pembroke Corgi.
I’m sorry for your loss.
I am also sorry for your loss..I am sure it has been heartbreaking.
hemangiosarcoma is a genetically based cancer and it is not the same in all animals. This particular cancer is not known in the coton de tulear. While I can’t say the Epi-Soothe caused my beloved pet’s illness, I can say that I believe my Abby was doing as well as could be expected after the homeopathic remedy was administered. So I believe this Virbac product definitely played a role in my dog’s succumbing to his cancer. You can google “DEA” and you will find quite a lot of information on this chemical as a carcinogen. This chemical is the second and third ingredient in Epi-Soothe.
I feel I am having a difficult time – less because my beloved pet died – than because of the fact that I used this product on him unwittingly and trusting in my vet to provide reliable advice. So I appreciate your support but I am not sure you get where I am coming from. I care about animals and the value of the love they give us…in return we put crap in and on their bodies and then feel sorry for ourselves when they die. It is big business in America and around the world. Dollars have more value than life…really?
Another thought, humans are given hospice care and often treated with powerful narcotics such as morphine to keep them comfortable. Animals, not so much.
Unless you have megabucks and can afford to hire a private nurse for your pet….then, maybe you would have more options.
I guess you are right …these might be the circumstances when euthanasia might be necessary. That is why I spent 3 hours in the vet’s office consulting with our homeopathic vet by phone desperately trying to determine what to do; running tests to try to figure out what was going on. Very reluctantly did I agree to euthanasia…I was told that Abby might die at home that night if I took him home. I was very afraid of prolonging my pet’s agony. When the anesthesia was administered, my sweet Abby died quickly. The vet told me that quick death from euthanasia is what happens when death is imminent. So maybe I could have given pain meds and then my sweet Abby would have died naturally a few hours later.
My biggest regret is using that terrible Virbac shampoo misnamed Episooth on Abby which was described as to me as an “oatmeal” bath. I am normally very careful about products but I was in a very fragile state myself from the stress of caring for an ill pup. I trusted the rehab vet to give me reliable information because some of what she was recommending seemed holistic – i.e. pet cancer diet, massage therapy, putting yoga mats down (I bought 12 mats that I now don’t know what to do with) …only to find out Episooth should be identified as a carcinogen…it probably contains less than 1% of soothing oatmeal; 2 of the first 3 ingredients are variations of DEA. After Abby’s death, when I googled this Virbac product, I found the article by California Vet, Patrick Mahaney, describing this as a carcinogenic product. Given the sores on my poor Abby’s head that appeared after using this product, it seems plausible that Episooth is a carcinogenic product that should be banned. Would any decent person recommend using a carcinogenic product on an animal battling cancer under homeopathic treatment? I have to believe that this is a product that is being heavily marketed to veterinarians. I am thinking of filing a lawsuit for infliction of emotional distress…no company should be able to profit at the expense of the health of our wonderful companions.
It’s not that simple, some animals suffer greatly and there are no pills or remedies that can stop the pain and discomfort. With hemangiosarcoma that has spread to the lungs for example, the large blood filled tumors start to burst making it extremely painful and difficult to breathe…..this can sometimes occur slowly.
In some ways, losing my Abby has been more painful than when either of my parents died. Abby weaved his way into my heart and gave me the will to get out every day and do what I needed to do. My son is disabled, I went through some really difficult times with his issues. My dog gave me the will to struggle through to do what I felt I needed to do. Abby’s love was unconditional and gave me the peace that nothing else could. I felt like I was finally able to start to plan to spend more time with Abby when he was diagnosed with cancer. I guess I have to accept that I never owned Abby; he was a magnificent gift of God’s creation. I loved to hold him on my lap and look into his soulful eyes while playing with his paws. Abby could not have been a better companion.
I thank Dr. Falconer for addressing this topic of euthanasia. I questioned whether I had done the right thing to euthanize…should I have let Abby die naturally? It weighs on me; we typically do not euthanize humans so why do we do this with animals who have become like family members. We need to respect our pets for the wonderful blessing they are; our pets are not objects of convenience. As we discuss this topic, I sincerely hope that knowledge will advance in such a way that will lead to improved quality of life for our furry friends. We humans need to learn how to be better shepherds; the natural end to life is much easier to accept when our pets have had the opportunity to live their life to the fullest. I agree that euthanasia should be performed in very limited circumstances.
This is such a tough decisional We have made it several times and maybe waited too long. it is so tough to let go. Both times, we waited till our dog seemed to say…Mom…had ENOUGH’ let me go. First time, my hubby did not want to stay with our dog so I bowed to his decision and left our precious dog with the Vet. NEVER AGAIN, NEVER AGAIN. I am the mom..i’m staying with our dog so that he knows he is safe…mom is there. The next time…We had the vet come to the house…We had spent the day with our dog (German Shorthair Pointer) and he had had a whirlpool bath (he love those) and was laying on the back porch with us on his pillow. Lovely day…He’d spent the last 6 months suffering from paralysis of his back end…not total…but he could not walk so we bought wheels from Eddie’s wheels and it did give him some life. but finally, we knew it was time. the life went out of his eyes..as if to say…Mom…i’m done. Had to let him go. so we just made it as easy as possible and …then he was done. Still cry when I think of it and as I do that, now…my current GSPs are looking at me wondering why mom is crying. Geesh. I’m sure blessed to be love by these dogs and my main hope is to take the best care of them that I can. I guess the point of this was…we take the cues from our dogs…what is their quality of life? will it improve? are they in pain? A friend also told us…when we have to let them go, it is the last good thing we can do for them….it’s never easy. we love them so.
Good post, I am highly tuned to what my pets need and when they are in pain or discomfort and if it is “time” to say goodbye but even so, I don’t always get it right. When we are dealing with love and grief, sometimes our judgment gets clouded and this is why we need a veterinarian who is not in a rush to end things when the animal is clearly still fighting to stick around. I allow my intuition to guide me and that requires getting my own heart out of the way so I don’t cloud my judgement. I think we all have the ability to connect with our pets on such a deep level that you will be able to “hear” their wishes in a calm peaceful state. It is no different than a mother intuitively knowing when their child has been injured or a spouse is in danger. As long as it is not an emergency situation and my pet can “talk” to me, I let them tell me when it is time.
Back in Nov 2014 my English Shepherd passed away on his favorite bed with me by his side. I saw it coming for the months before that. The hind end weakness cause by a neurologic event he had a year prior. He was one of those who would not go in the house no matter what, but it starting happening and I know he felt horrible about it. It was taking alot of work on our part to keep him clean. He wasn’t sleeping much anymore, didn’t hear well anymore and his mind seemed to be going. Then one Sunday my husband helped him out to pee with the help of a carrier under him back end. He walked very slowly the whole parameter of our back yard fence, stopping and smelling along the way. We we got him back inside on his favorite bed he just lay there kinda off in the distant. I had a animal communicator speak with him and he told her his time was very very near. He said he thought he would need help with crossing. At this point it was late in the evening and I didn’t want to take him to a unfamiliar place and my reg vet was closed. It was a restless night but I had given him some pain meds and that seemed to help. He crossed by himself early the next morning. I still feel guilty about that but the communicator has since spoken to him and he is happy and glad to be out of his body and said everything is good and glad that I was with him. Miss that old man but going the natural,holistic route has helped me be ok with this because I now understand the natural process so much better. Thanks for letting me get this off my chest 🙂
I would love to connect with an animal communicator. How were you able to verify the authenticity of her work?
We lost our older Heeler a few weeks ago. He was 13 and a few months. We were wondering if we were getting close to a time we might need to consider when was the right time to “let him go”, not wanting him to suffer. He was slowing down but no real indication of any serious disease. We had raised him according to many of your vital animal principles, using homeopathy and herbs, limited vaccination, keeping him out of the vet’s office, and other things, but I didn’t know you or have your newsletter until last year, so unfortunately he didn’t benefit from many of the things I’ve been learning since we got our new pup this year. But our dog “Blue” was the absolute best dog we could ever have had and we enjoyed him so much. It has led to us having a lifelong love of the breed and our new pup is a heeler too.
Blue was slowing down last year and within a couple weeks of his death wasn’t leaving his bed too much. One day I was particularly worried about him and sat with him most of the day just loving on him. I gave him some of the Bachs that you recommended to see how his vitality was and he did perk up for a few more days. My husband was always saying that he would never let Blue suffer and if need be, he would take him out to the country and take care of him “old Yeller” style. I never wanted that to happen. Blue waited for my husband and son to come back from a late year trip to Big Bend and then about two days later on his last day, he got up, went outside to the bathroom, ate his glucosamine treats and drank some water, and then laid down on his bed for a morning nap. We all left the house for a little while and when I got back, I found Blue had passed on his bed, hopefully in his sleep. I was shocked and also not surprised knowing how he had been slowing down. I did not think it was time or I would have stayed home with him, but when he got up that morning and also ate, I thought he was doing OK. I’m so relieved he had a natural death and we didn’t have to put him down though.
We will plant bluebonnets over his grave next Fall so that hopefully each Spring we will get a beautiful reminder of our best dog “Blue”.
Oh gosh….what a beautiful story, I take it you are in Texas, what with the bluebonnets, etc. I was raised there and this brought back memories….How wonderful that you did not have to take extreme action…that Blue knew it was time and slipped away. I’m sure you know that people usually try to slip away when THEIR people are OUT of the room…then the go. I wonder if it is the same for dogs…wait till you are gone, then slip away so that you don’t have to see them and they don’t have to know how sad you are. Just speculation on my part based on humans…there is such a close bond, wondering …Sorry for your loss. Been there too many times and have two more German Shorthair Pointers who, unfortunately, I’ll lose some day. the later, the better. They have my heart. Sniff.
Columbo, he was just shy of 20 years old, we rescued him when he was but 2 years old, he was full of energy as most pugs are, he had been in the pound more than out and it was time he needed a real home, one where he could be all he was meant to be.
Hubby and i drive truck, we already had 2 pugs our Tigger and her sister Black Banjo, but we could not turn our back on this rebel of a pug, he loved to run, so he became a trucker, and oh what a trucker he was.
He crossed many borders, made his mark on trees in every state, and made friends with every one he met, Columbo the Private Eye of Pugs, he was always ready to find what ever it was his nose lead him to.
At 7 years he swallowed some thing he should not have, the cap off the ready whip bottle, shame on daddy for feeding him ready whip, after 2 weeks it had not passed, so we took him in and an ex-ray was done, they could not find it, but they did find he had advanced hip dysplasia, he had never limited or showed any signs, we did not worry about it. (he puked that cap at week 4)
Our guy was healthy, we never had any issues with him, we had him on a good quality dry food, at that time i did not know i could feed a raw diet, and he got his shots every year as we thought was right, even tho Columbo had to have benidryl before every shot, when he turned 10 he had NO MORE shots, i was learning the danger.
We lost Tigger at 16 years, mouth cancer, and Banjo her enlarger heart took her at 17 years, but Columbo just seemed to never even slow down.
In January of 2014 i finally went total raw, oh he loved it, by this time he had been having a bit of trouble walking, the hip was going fast now, and he had a couple seizures, i added COQ10 and organic honey between meals, that solved that problem, his fur become softer than it had ever been, and he stopped drinking every 5 minutes, he seemed to do a lot better, he was with us for 6 more months, and then in July he just could not stand no more, he would not lay down and rest, he howled when i left the room, it was time.
He fell asleep in my arms as we waited for the vet to come in, he was ready even if we were not, at just shy of 20 years we helped him pass, by far he was the hardest, with well over a million miles under his color he took the final ride, and we said good bye to the greatest pug there ever was, that rebel that was born to travel is now on the highway to heaven, where we will one day meet again.
good bye is never easy, but there are times when we have to let the tears fall as they may, because their life is worth more than a broken heart, it was and is worth every mile, and the joy of his memory quickly filled the edges and healed that broken heart, because of him we will always be better than we were before he came.
Good Bye for now, but not forever!
Columbo was one strong constitution-ed guy, Mandy! Not many pugs I’ve ever met made it to 20 years old. And he made it very clear when euthanasia was appropriate.
Thanks for sharing his story with us.
Important topic! Thank you, Dr. Falconer and thank all of you who’ve contributed your stories.
I, too, believe that many times, the suggestion of euthanasia after a diagnosis is more for the people than the animal. There is a time and place for euthanasia for both people and animals but each should decide for themselves. And we can tune in to our animals to get their message to us.
In this society it seems that doctors have to make those decisions for humans and why is that! Also, relegating the decision to euthanize our pets has been strongly influenced by the doctor’s suggestion. My feeling is that we need to take back our power from the so-called experts. They’re good at diagnostics and they’re good at putting together broken bones and stitching skin together, but curing the illness, definitely not.
One thing bothers me as I read people’s stories. Why do we agree to amputate our pets’ appendages when there is cancer? Even after cutting it off, the cancer still remains in the body and shows itself somewhere else later. The only legal protocols for cancer treatment are surgery (cutting out the offending tumor or infested organ), radiation and chemo. Not only do those protocols not work in the long run, they are downright barbaric not that far removed from the blood letting and other horrific medical protocols of the 19th century.
Conventional medicine compartmentalizes illness or disease without looking at the person or pet as a whole and that’s where they are way off base. You can’t just treat one part and be successful.
I’m looking forward to hearing stories from folks who’ve never vaccinated, feed species appropriate foods, use homeopathy, and provide plenty of love, exercise, fresh air and sunshine to see if their pets ever experience cancer, digestive issues, and other similar diseases.
Thanks for your time reading my ramblings.
Hello Elle!
Just my thoughts on amputation of Bella’s leg. She was extremely healthy and so very active. Leaving that leg on her would have created her to become unhealthy and with no activity. Remember it is quality of life for them. Why leave her miserable with a painful cancer growth in her joint when removing it took away the pain, the gimp, the swollen balloon that developed and then allowed her to be with us another year and a half. Yes, I too thought it was barbaric, but what alternative did I have. What I felt was more barbaric was letting that cancer fester within that joint and then watching her eat at her leg as I found her doing to her remaining leg that developed cancer, on the day I had to decide it was “time”. She received no chemo with the removal of the first leg and she continued on with all her supplements, however we added bosweilla to her regimen that she was never on. Painkillers were never needed until it moved into her remaining leg. Yes, she received them for the first week after surgery, but that was it. You would have never known she was on three legs. Most times, animals are stronger than humans as I watched in both my loved ones that have passed on. I suppose we are all different in what each of us can handle. We all have different opinions on how matters should be handled and until faced with each of our circumstances you mustn’t judge the decisions others still have to make and have made. Bella had a great life after that leg was removed. I hope anyone reading this understands, if faced with a bone cancer issue, that if the loved one is of good health, they can adapt and move on with life without that limb. God Bless! RJ
Well put, RJ. Surgery of a bone cancerous limb is properly viewed as a pain-sparing, quality of life enhancing procedure.
I suspect it’s also viewed all too often as part of fighting the cancer, which, as Elle points out, it’s not.
It can have its place, and as you rightly relate, dogs do exceeding well on 3 legs. You can even see some on Youtube who do amazing well with two legs.
I agree …I am very troubled by the fact that so many dogs getting cancer. I saw that hemangiosarcoma can be caused by arsenic and I wonder if there is arsenic in the food we are feeding our beloved pets. I have read where arsenic is in rice and pet food products very often contain rice. My dog, Abby, got colitis in March 2014, prior to his decline and finally his cancer diagnosis in late August. He had been treated with antibiotics for the colitis and in retrospect I now believe those antibiotics may have spurred the growth of what may have been a slow growing cancer as I have read that hemangiosarcoma can remain relatively dormant and then start a rapid growth. Let me also add that I take euthanasia very seriously – several times the topic came up during the 4 months leading to that fateful decision on Dec. 25th. I would never euthanize unless I felt it was absolutely necessary for my dog…I am truly going through a grieving process as I look back and wish that I had cared for my dog differently in a way that would have prevented this outcome. My dog was showing signs of stress in his last few years…I think it was the cumulative outcome of conventional pet care – not enough exercise – a less than optimal diet.
Hemangiosarcoma is one of the most horrible things I have ever witnessed.
Despite the best diet, exercise, avoidance of vaccines and chemicals, this nightmare thing happened to one of my dogs. Genetic link? Not caught early enough? Who knows….
My pup, Abby, was 6 months old when I got him…I often wonder if something happened to him before I got him. I adored his personality but he could be a bit hyper and was said to exhibit what was termed “fear aggression”. Now, I am just beginning to learn about homeopathy but one of the basic tenets is that serious illness manifests as the cumulative effect of lesser illness throughout the lifetime which is a product of the emotional state. Now, hemangiosarcoma is not considered common in the coton de tulear…it is interesting because an analogous illness in humans is hemangiomas which is not a cancer but I have a fair number of hemangiomas on my skin. I have to wonder if something in our relationship could have impacted Abby’s illness.
I am so sorry that hemangiosarcoma struck your pup despite your best efforts…I do believe there is a genetic link to this illness…I have another coton from the same breeder as Abby and there are common ancestors in their family tree. But it is interesting because personality wise – Abby and Lars are very different. Lars will be 13 in March so I am now on gurad with him. Now, I am trying to contact the breeder in Sweden to see if she has seen this illness in her other pups. I just mailed her a letter today,
I refused to follow my vet’s suggestion to euthanize my cat, Pookie after an April 2014 diagnosis of an abdominal mass. Instead we started her on Venus Fly Trap, blue/green algae, krill oil and a dozen other things, including daily sun baths, probiotics, purified water and colloidal silver.
She returned to Dr. Whitecoat last week for a thyroid test, and he was amazed that she was not only still alive, but she had gained two pounds. It’ll be a year soon since her diagnosis, and her tumor hasn’t gotten any larger. Her vomiting and constipation have been resolved, and she is continuing to improve, at the ripe old age of 12 yrs+9 mos.
When it IS time to say goodbye, which I hope is years off, it’ll be hard to let go of the life I’ve fought so hard to extend. The decision will not be made lightly, unlike Dr. Whitecoat, who doesn’t understand the influence of positive energy and love on illness, but plays fast and loose with that precious life with his cut/poison/burn, “it’s hopeless” model. If she isn’t crying out in pain, I believe she should be given every opportunity to live a happy life for as long as she’s able to, draped across my lap where she belongs, tumor and all. After all, it just might disappear!
Nice, Nora. You’ve clearly made some amazing progress with your Pookie, contrary to what was expected in conventional circles.
My beautiful golden broke her leg walking in the yard, I rushed her to my vet and then on to specialist. The next day they
Began surgery, they called me and said they werr sure it was cancer but could not be positive until results csme back, they also felt it would be somewhere else in.her body. What did I want them to do.
I was beyond knowing the best thing for my 12 year old girl, I callef my vet snd he recommended
I guess I’ve been lucky, if you want to call it that, that I haven’t had to make the decision when I’ve lost three dogs. Shadoe was in the latter stages of bladder cancer in 2002, and on the days I’d made appts to end his suffering, he was happy, eating, enjoying life so I was able to cancel — twice. With a friend’s help, I treated him with coenzyme Q-10, venus flytrap and a collection of tinctures I can’t recall, from August to January, surprising our vet that he lived that much longer post diagnosis. On a Sunday evening, convulsions and panting began — it was obviously time. Only two days ago, he’d wanted to chase a cat. He’d had dinner that day, but left a bowel movement in the kitchen, something he never did, which we found as a parting gift when we returned home after letting him go.
A few weeks later, I added two puppies to my life, brother and sister Summit and Hillary. I lost Summit just short of 10 yrs to bone cancer in 2013; Hillary just last November to hemangiosarcoma. Having kibble-fed Shadoe, from the time they were 6 months old, I chose to feed them raw, home-made meals. Vaccinations were minimal — only three of each of the main ones over the first nine years of their lives. Still — the Ugly C stepped in. Summit was a shock, as I’ll explain. The time to say good-bye to Hillary was obvious. Although shocking to lose her in just 24 hours, I understand that is often the case with HG. It wasn’t diagnosed so we enjoyed a year of blissful ignorance, not knowing what was ahead. She ate, played, went on walks, visits to the park, car rides, bossed around the younger dogs, came to work and just enjoyed life. As her body rapidly gave up, there was no question but to help her leave this world. Sad, but with no regrets.
Until Summit’s illness, both were healthy, happy and active. Checkups were uneventful. Like my own health, we didn’t have issues so there was no need to be up-to-date on the latest holistic and natural treatments. We ate well and lived well.
So when Summit started limping, and at the end of that first week I took him in — and received the horrific news that it was bone cancer, I was stunned. I had no backup. Only the oncologist’s direction. The Guelph University Veterinary Hospital, one of the finest, I understand, did a comprehensive screening process — x-rays, ultrasound of organs, and bone scan. I cried tears of joy when I was told each successive test showed no other cancer (understanding that metastasis was still possible later) and that he was an excellent candidate for amputation. From discovery to the surgery was 13 days when I tried to find success stores, support groups and miracle solutions. There was so much to read and so little time. I was grasping but couldn’t find the answers or sources I needed.
What I know now is that he wouldn’t have suffered or gotten any worse if I’d taken more time to research and talk to others–a few weeks or a few months if needed. I too was told the leg could fracture. Surgery was strongly recommended. I’ve since learned bone can strengthen and even regrow. A friend I met has X-rays showing this in her Rottie. And yes, her vet was impressed, the same vet that told her it was inoperable and she only had a few months to live. She went on for 24 months of healthy, happy living. I’ve found bone cancer groups and groups that advocate artemisinin and other courses of immunity support. I understand the importance of strengthening the body, the organs and the immune system. That cancer can be held at bay. That months can easily (well, with lots of hard work) lead to years. That homeopathic methods are a way to strengthen a system stressed by cancer and amputation.
I didn’t know all of this then. Instead I rushed to cut out the cancer as advised. I felt helpless. The only thing I could do when I brought him in for surgery was bring several meals of doggie chicken soup so I could avoid the Purina meals I was worried they’d feed him, but I can’t be sure he was fed them. 🙁 Against my better judgement, as I didn’t have any research or an alternative or success stories to fall back on, I allowed chemo. Summit was miserable on chemo. He’d no sooner recover his strength and it was time for another dose. Three months after surgery, when making an emergency trip to Guelph because of his lethargy, Summit died enroute. Sadly, I didn’t have to make the decision for euthanasia this time either. An infection did that. An infection caused by a weakened immune system most likely from the chemo.
It’s my belief that when he suffered through the chemo, he was actually fighting an infection that worsened with the presence of chemo. No one was looking for an infection, they expected his immune system to be diminished. They ignored the patient. It wasn’t normal to have a reaction to chemo 2 weeks later, but that was ignored. When his white blood count was elevated, they’d wait for it to normalize and then administer chemo. They didn’t look for infection. They ignored that as they were treating bone cancer, not the dog.
Three and a half years later, I still follow and support caregivers of bone cancer dogs, sharing my story, offering support when they receive a dire diagnosis and a death sentence. I now have the success stories. I have lists of things people have tried that have given them more days, weeks and months with their dogs. I share the info I’ve learned from others so that those that don’t think they have time for research can see another side, hear some success stories, hear about alternatives that offer quality of life. Then when they hear the diagnosis, they are prepared in a way I was not. I know that had Summit lived longer, I would one day face the euthanasia decision — it’s a decision I would have gladly made later rather than losing him so early in the battle.
Wow, Joanne, what an inspiring story! You’ve taken lemons and made lemonade that you are sharing to help others who could benefit from your path with Summit. Bravo.
Hi Joann, Your story of your Summit has really hit home with me. My sweet almost 8 year old black lab was diagnosed with osteosarcoma 2 weeks ago. He had been limping intermittantly for a good 8 months. I’ve also seen an oncologist, tried to do research on the internet and feel like you felt. I’ve decided on palliative treatment but am feeling pressured into amputation. I’ve been on the Tripawd website trying to muster the strength to move forward with it, but something keeps holding me back. He is handling painkillers very well…no constipation, good appetite, and actually is in better spirits than before his diagnosis. I want him to be comfortable in his remaining time here with us. From everything I read, all of those treatments aren’t giving the dog a much greater survival time. You mention artemisinin, what is that? I’m writing to you because you say you’re involved in supporting those of us whose dogs have received this awful diagnosis. Thank you in advance for any info you are willing to share. Lisa Baird
I lost my Shepherd Charlie in August 2014 to DM. As you said, he was normal from the waist up, but completely paralyzed in his lower half. When he could no longer control his bowels, I adopted a little dog to keep him company as he now had to live outside during the day where I could clean up after him easily and he could move around on his own. Thankfully, on a raw diet his poops were not messy! He slept inside in the laundry room at night. He was happy and had a good appetite. Then one night I could see he was in distress; it was time. From the time he was diagnosed to the time I had to let him go was 3 wonderful years. Those 3 years were priceless to me. I feel when we make the decision to care for an animal we are responsible for them until the very end. Pets are not an old piece of furniture to be destroyed when they have outlived their usefulness. Friends who saw his paralyzed hind end said I should put him down. But, he still wanted to live and with the help of a wheelchair, he could still go on his walks. Everyone has to make their own choice, but I am glad I helped him to enjoy his life to the very end.
Three years is nothing to sniff at, others’ opinions aside. Thanks for being there for Charlie and sharing his story, Lori.
Thank you for your kind words. I believe the raw diet, electro-acupunture, wet homeopathy and laser treatments truly contributed to his 3 years after diagnosis. From my research, most DM dogs do not survive this long.
Hi Dr. Falconer,
Your past patient and my sweet companion of 12+ years, Moka died a little over a week ago. As you know, she was a perfectly fine puppy until she got her round of 2 year vaccines – then, over time, she developed horrible allergies, ear infections, bladder infections, huge lipomas, and skin staph infections. I started researching and realized that it was probably the vaccines that caused her ill health. I tried some TCM for a while but it didn’t seem to help. Then you guided her care for years. She never came back to being a healthy dog, but I do believe the homeopathy made a positive difference in her quality of life.
Luckily she was fairly normal until the day before her death. That morning she drank a LOT of water and was very picky about eating her breakfast. She seemed OK that evening when I got home from work. She woke me at 3:30 in the morning with a retching sound. When I turned on the light she had her legs straight out and her head thrown back. After that she was very weak. I took her outside to see if she needed to potty but she just stood there. When she did walk she wobbled. Her breathing was also labored. I just put her in her bed beside mine and watched her until I could take her to the vet. I had to get up and go potty myself at one point. When I came out of the bathroom she wasn’t in her bed. Even as she was dying she went outside via the doggy door to go potty. She had collapsed in the yard. I scooped her up and brought her inside. We sat down on the kitchen floor and I was able to pet her and repeatedly tell her how much I loved her for the last 10 minutes of her life as she finally gasped about four times and passed in the arms of her “mommy.” I have no idea what caused her death, but I’m thinking it might have been a heart valve issue like her sister, Biscuit, who died 2-1/2 years ago. I’m just glad she could die at home with me and that I didn’t have to take her to the vet (a place she did not like). I’m also glad I didn’t have to make the decision – she made it for me.
She was a daily source of blessing and joy to me for over 12 years and I miss her terribly. This forum seemed a timely way to let you know of her passing. Thank you for your years of trying one thing and another in an effort to bring her closer to being vital. I really don’t think she would have made it 12 years if it hadn’t been for the homeopathy.
Hi Marcia,
I’m so sorry you lost Moka, but grateful you could be with her to comfort her transition. I feel your loneliness and hope that pain can be soothed and healed as soon as its time allows.
All my best to you.
Article: Playing Fast and Loose with Euthanasia – Dr Will Falconer DVM
After reading this article I would like to convey my condolences to those, on the loss of their beloved pet. I also appreciate and value that you wrote this touching article on Euthanasia, in reference to Irma, the senior Golden Retriever, Dr. Wil.
My cat “Renoir”, also known as Cat-Man, lived to be close to 17 years old. In his final years, he was diabetic, and had bad teeth. He shared our humble abode with 2-wolfhounds, who Cat-Man greeted every morning.
Cat-Man contributed vastly to our family group dynamic. In our quiet, happy home, our cat would sleep most of the time, but would still swagger to his food dish, and tease the hounds, to say “I’m the boss”. – He was.
Cat-man got a tooth infection, which was treated with medication giving him a diabetic crash. Poor animal, I was unsure which end it was going to come out. Tough cat, he survived, though we both knew his days were numbered. We shared our days together, for as long as we could.
Cat man lived for another 6-months, until our last day together. He could no longer swagger up to the dogs to tease them. He could no longer stand up, and he looked at me – I understood.
Dr. Will once said sometimes we walk a lonely road, if we stick to our guns. My neighbors chewed me out for being selfish, cruel, and I won’t repeat the rest. This is for not putting him down after his immediate diabetic crash, when he was ill with the infected tooth. He’s old, they said.
Neutrical helped him from his diabetic crash, and I nursed him better, to live for 6 more months. It was not his time to leave regardless of what anyone yelled at me. I do not put my furry pal down until he lets me know it’s time, despite the Poo-Poo of the neighbors. My cat showed me who my true friends are in his passing days. Cat wisdom at its finest. – He’s the boss.
Condolences to all who grieve after their beloved furry friend, I still miss Cat-man too. In the silence of our last moments together, I learned cat-wisdom yet again. It is to know and understand by listening to your heart, it does not lie to you.
We’re different because we establish stronger bonds with our animals and we strive to know more, understand them better, and we read more.
This is also what Dr. Will nicely describes in this article. Don’t listen to them, only you and your animal will know regardless of what they say. Thank you for writing this article Dr. Will.
JP
Since I became a homeopath 15 years ago, I have only once had the need to euthanase any of my not inconsiderable menagerie, and that was a horse who was down. When their time comes, their natural life (good diet, holistic medicine) allows them to die as they would like to. Yes, I think it can be useful, but it is used far, far more than it is necessary. I believe it is more for the people than the animals.
Our stress does add to their burden, too. We all choose our time of birth, so we can our end, too. My dogs and cats have shown they are coming to their end by slowing down, then not eating. Then they die in their sleep. I want to go like that!
And of course, there are the wonderful homeopathic remedies that ease pain and fear allowing animals to either jump back into life or die peacefully. One cat person called it ‘my magic potion’! Death is not the end, it is not to be feared. It is a transition, like a caterpillar transitioning into a butterfly. Life force is energy and you cannot destroy energy, just transform it.
What a beautiful description of the end of life!
I learned a long time ago_the hard way_to be very careful in trusting “traditional” veterinarians. …about the same with “traditional” human medical doctors.
It appears to me that Dr. Falconer takes every factor into consideration. I bow to him for that. There are many factors to take into account and each patient is as unique as it’s owners. Everything has to be considered_with the help of a compassionate veterinarian.
I had an adult male cat years ago and noticed his left hip protruded a little more than the other. I asked the veterinarian to get an x-ray and he said it wasn’t necessary_just normal_maybe arthritis. I tried to tell him I “knew” my own cat and would really like an x-ray. Well, a year later, Sugar Plum started having bowel movement problems. After many trips to the same veterinarian and enemas each time, I requested an x-ray. The younger veterinarian said it wasn’t needed, but I insisted. When I returned for the results, he informed me that he was glad I insisted, because Sugar Plum had bone cancer in that hip and it was compressing the colon. He said amputation would be too dangerous at that time. I refused their offer of euthanasia and just took care of him the best I could.
I moved to another city and found a veterinarian who respected my decision and helped me use more “holistic” or “natural” ways of caring for Sugar Plum. It got to the point that Sugar Plum needed IV fluid too often. He was just slipping away. The veterinarian and I talked and I decided I might not bring Sugar Plum in for the next IV. He was honest enough to tell him he didn’t like to keep sticking him_when it just prolonged and didn’t cure. Most veterinarians I knew would have just continued_to make the money. The veterinarian told me to call him day or night, if “we” needed anything. I will never forget that and am forever indebted to him for his compassion.
Sugar Plum lived a happy life for a year after that x-ray. He passed away soon after the last IV fluid. I’d always walk him with a soft harness in the apartment complex courtyard. He loved climbing the mesquite tree. A few hours before he died, I took him out and laid him in the grass he loved so much. Laying on his side, he sniffed the earth and grass, then looked into my eyes. I really believe I saw his little soul in his eyes. I petted him awhile and then took him back inside. I put him on his pillow and sat with him, until he finally took a deep breath and left that little body behind.
I am so happy Dr. Falconer wrote this article. He reminds me of how impermanent life is and to appreciate every moment. I miss Sugar Plum. We buried his body, but not his mind-stream. I hope he is happy and well and may ALL be happy and well.
My puppy had a reaction to the rabies vaccine. Only rabies vaccine I’d ever given to a dog and the only one I ever will, as it’s not required where I live. At six months the vet noticed that she looked bloated. It came back that she was collecting fluid in her abdomen for an unknown reason. Many tests later and hundreds of dollars I had still had no answers and the vet suggested euthanasia.
I did think about.
But then I thought about how SHE felt.
She came to greet me everyday when I came home, tail wagging. She loved her toys and her food, maybe a little too much, but all the same. And boy could that dog move when she wanted to! Even when she ballooned to twice the weight she was supposed to be. She was a spunky (w)itch who would kick butt and did so. Nor would she let anyone forget it. When I got my second dog a year and a half later, it was her way or no way. She was never mean but she certainly was a handful up until the time she left us at five. Four and a half years after the vet wanted to put her down.
And then the vet did me another injustice.
She got ill quite rapidly, and judging from her symptoms I figured she had a blocked intestine or that they had finally twisted. (One of the test when they were trying to diagnose her at six months was an ultrasound and it was quite clear the intestines where flipping around freely.) I did tell them what I suspected.
They ran a bunch of tests and kept her in for the night, giving her fluids. They called me in the morning and told me she was already to go, that she’s stopped vomiting. I picked her up. I didn’t even get home before the vomiting started again.
She passed soon after. At home. I have not forgiven them for lying to me. I have a feeling she just buried the vomit in those blue pad things. She was a smart thing with a will of iron. Three and a half years later the other dog still does the odd quirk she learned from her, always makes me smile.
Hi Paula,
Four and a half years is quite a run. You were doing something right.
And I’d hazard another interpretation on the vets sending her home. Rather than lying, it’s more likely her symptom of vomiting had been suppressed with a drug. The effects wore off and you saw the symptom return.
Thanks for sharing her story with us.
Hello,
My beautiful and cherished Abby was euthanized on Dec. 25, 204. It was an agonizing decision that came after a cancer diagnosis in late August. At first, I was paralyzed with fear – my poor Abby’s hind leg was amputated on Sept. 4 2 days after an oncology consult. Later pathology showed hemangiosarcoma which typically begins in the spleen. Then my poor Abby’s suture site became infected possibly due to an ill fitting soft e-collar and required 2 invasive procedures to fix. We then again consulted with oncology who did ultrasound that showed metastatic cancer. At that point, I decided to consult with homeopathic vet, Sidney Storozum instead of going the chemotherapy route. Subsequently, I thought Abby was doing well so I wanted to work with a rehab vet to be able to take Abby out for walks. That rehab vet (who works in the same facility as the oncology vets) recommended EpiSooth shampoo for a mild irritation on Abby’s leg. I ordered the Episooth and Abby developed a sore on top of his head after I used it to bath him. Abby began to deteriorate rather quickly in late Dec. On the 25th he was breathing rapidly and had reduced perfusion. We took him to a vet to be checked. As we sat there in the vet’s office it became apparent that Abby’s cancer had likely spread and he may be going into shock. He laid down on his side and cried out rather strongly. He was no longer drinking water. As difficult as it was, I agreed to the vet’s recommendation to euthanize my beloved Abby. I feel some torment – She said Abby needed to be seen by cardiology ASAP. No one was available until the morning. So I sometimes wonder if Abby might have been saved but it is not likely. It would have given me more closure if his heart had been checked.
Looking back, I learned that EpiSooth is banned in the state of California because it contains the carcinogen DEA. This information greatly upsets me because I bathed my dog in that product per the recommendation of the rehab vet and he later developed a sore on his head. Some other sores were apparent around his mouth just prior to the euthanasia. At some level, I wondered if the recommendation for the Episooth was a deliberate attempt to sabotage Abby’s homeopathic treatment. I know that is an awful thought but it has left me feeling really distrustful of conventional vet care.
Hi Susan,
A difficult death decision, yours. I’m so sorry for your loss.
What is a safe shampoo for my doggies? I just read the previous e mail and quickly trashed the Epi Soothe I has purchased at my vet. My dogs eat all raw, organic food. Thank you for your help. I am in Dallas.
Sammie Smotj
Hi Sammie,
There are a lot of choices these days. I no longer carry one, but I’d take a peak over on Dogs Naturally Magazine and see what they have.
Thank you so much…It was not easy..I am not sure if Abby was incontinent but I was really struggling with clean up. Also on the 24th of Dec, it seemed that Abby’s vision was going. Abby kept getting caught in places and I kept rescuing him. All around, it seemed like Abby’s health was failing…I was reluctant to put him on pain medication knowing the side effects of constipation which he went through after the leg amputation. I felt like Abby was telling me he needed to go. His death was quick and peaceful.
I am trying to stay focused on the plus side of things. Abby and I had 15 1/2 wonderful years together …it was only when he was diagnosed in August that I realized how much my pup enriched my life. He gave so much and asked for so little. I try to imagine him in heaven reunited with his canine family.
Dr. Falconer, funny you should touch on this subject after I wrote in earlier about the rabies controversy. Bella, our chocolate lab….age 6. She started gimping as though she had something in her foot. I thought could she have arthritis at such a young age. Sure enough the x-ray came back positive for bone cancer. What were my options, as I did not believe in euthanization, I always felt it was not my decision it was God’s. I watched my grandma die from liver cancer and morphine became her best friend. The homeopathic vet told me remove her leg, she is healthy and happy and it may give you a year, five years or more with her. I went the next day, praying it would be another ten years we would have her. I cried hysterically when the vet brought her into the room to us after surgery and then thought to myself although she looked odd because of my decision, she walked all on her own to me, wagging her tail as to say what are you crying about, trying to comfort me when I should have been comforting her. We had her a year and a half and during that time she was active, still could outrun any of the other dogs we had and still protected us and anything of ours. But one day she started gimping on the remaining rear leg and it began to swell. In my mind I knew what it was and had researched and resolved myself that we would have the rear leg removed and put her on wheels. This time we took her to Columbia veterinary school of medicine and it was there the fateful x-ray showed the bone cancer had metastasized to her lungs and was also in the joint of that remaining leg….huge tumors had filled her lungs and I also knew this could happen and in 90% of the cases it does and it is the lung cancer that takes them before the bone cancer. We took her home with a script of tramadol. She still was able to eliminate on her own outside, but we had to carry her there…she had a ravenous appetite and still wagged her tail a little bit. I prayed for the Lord to take her, but He didn’t He made me make the decision. It happened one day, two months after that last x-ray, when I walked in and to my horror, found her eating her leg where the cancer was. It was time, she knew it was time, I still was in denial, but on that day she brought me her bone all on her own and laid down by me wagging her tail. It was okay, as I sit here crying, still to this day, that she was trying to tell me it was time to go. It’s the only way you can view such an emotional decision. It is so hard and something nobody ever wants to do. With life comes death and it is the enjoyment of life and those memories we make with them that helps us pass through death. We love her, will always love her and smile when one of our furry loved ones do something she used to do. May the Lord comfort everyone who has to endure such a difficult decision. God Bless to all! RJ
RJ, what an amazing request this gentle creature made of you. No clearer, “It’s time,” have I ever heard. And still the good dog till the end, wagging and all.
My condolences for your loss. And my thanks for sharing this amazing story.
RJ, I am sitting here, tears streaming down my face, reading your heartfelt story of Bella, as I am still mourning the loss of my 6 yr old Max who passed this past May, as I miss him so very much….I am crying for us both. May God bless you, and all of us whom are missing our pets.
Bonita, it is so very difficult and there are days the pain comes back so intense and as though it had just happened all over again. But, the Lord gives us so many orphaned, furry loved ones to choose from to heal the pain we suffer with each day from our loved one that passes and that helps, along with time, to heal the emotional pain. God Bless to you! RJ
I don’t have any words…I am stunned and amazed. I am deeply touched and humbled by your loss. What a courage and strength of your dog. You have my deepest love and condolences.
Thank you Julie. Bella was a tremendous animal. She was a rescue dog that came from Kentucky. She, her brother and mother were found on the highway…Bella, of course, was a pup. The mother had tags and the vet who found them took them back to the owner. They told the vet, we’ll take the mom back but we’re just going to kill the pups, as they both were the runts. So, Bella made her way back to Illinois with a college friend of our daughters and we took her from there. She was a fighter from day one….with a mission….to teach us how much love a rescue can bring to the family…she was our first rescue, our Sunny was a breeder pup and we had all the documents to prove it LOL and yet there wasn’t a lick of difference in either of them….rescue versus pure bred…they both gave so much to us all and one day we will all be together again. God bless you and thank you for your thoughts! RJ
Hear Hear, Doc.
I first came to you as a human and her feline patient upon hearing “you just picked this cat off the street and had him neutered and plan to keep him safe in your home, but he’s FeLeuk+, so you should just put him down. Oren had 4 magnificent thriving years with me under your care (he was a middle aged street cat when I took him in). He was a magnificent animal, and I am still gutted that he left me when he did. He was well until he wasn’t, and it came on very fast.
And then, there was dear old sagely Franklin. I was in no way planning to euthanize him the day that ended up happening, but that evening, after I got home from work, it washed over me that he was only here because he thought I wanted/needed him to be. He had stopped eating, and moving around was very difficult for him. He was very weak. He just laid listlessly, feigning interest if I called him. In that instant, it came to me that we/he didn’t have to do this anymore. I had to help him in and out of the car that night– that was the ONLY time I ever had to do that for him, and he was not pleased about it. “Mom. Hey. I do this on my own, remember?” …only, he couldn’t. His disease had progressed to where he didn’t get to live on the terms he had so perfectly set for himself for 15 years. Even though he wasn’t in any apparent intractable pain, and incontinence wasn’t an issue, and the explosive nosebleeds that came with his cancer had also been controlled to some extent. In his case, it was just a gentle wave of acceptance that he didn’t need to starve to death, which is where he was heading over the next few days. You and I were emailing that night, and you wrote, “if he’s no longer eating, then drinking will be next, followed by loss of consciousness.” When I realized that’s where we were, and he was clearly on his way out, but felt he needed to be there for me, I set my friend free.
We aimed for a gentle landing, and he definitely had that.
I will never ever understand vets who suggest euthanization based on diagnostics. I mean, we don’t ever even consider that for humans (even when there IS intractable pain and zero hope of healing), so why on earth would we suggest doing so simply because the patient isn’t verbal (let me be clear– verbal as in human speech)?? Makes zero sense to me. How can someone call themselves a doctor and not honor the sentient nature of their patients simply because they have 4 legs and bark or meow or whinney or whatever the vocalization may be? Beats me.
Thanks for writing this.